
ORX RISK ANALYZER©
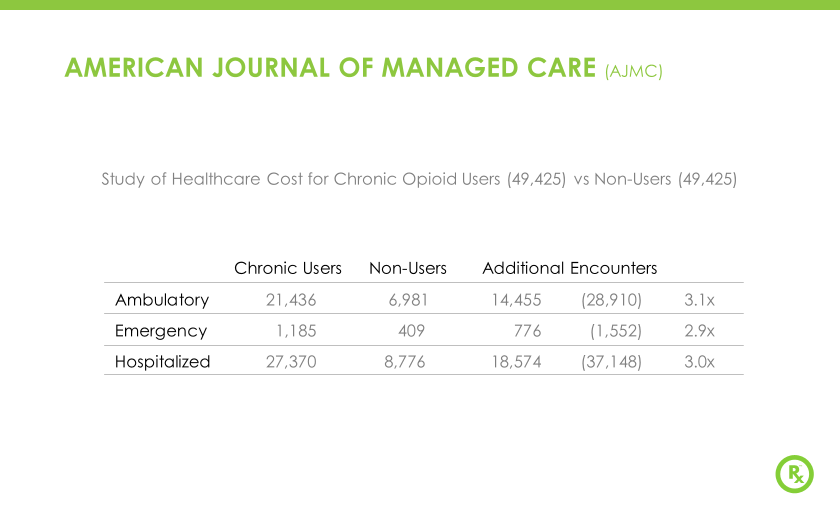
The ORx Risk Analyzer© retrospectively analyzes paid prescriptions of non-identified health plan members and identifies their prescription re-fill patterns. Utilizing predictive analytics, the ORx Risk Analyzer identifies Rx refill patterns that can be due to chronic usage, abuse, brain chemistry response and or other chronic medical issues. Research has shown prescribed opioids and usage patterns can cause 3(X) more healthcare encounters than patients not prescribed opioids.
The initial ORx Risk Analysis© provides the Prescription Compliance Report (PCR), which is a retrospective view of non-identified plan members. This analysis indicates the current prescription re-fill patterns compared to prescribed medications. The Prescription Compliance Report© (PCR© ) creates a base line of plan members, costs, providers and pharmacies that are providing chronic pain management with narcotic and opioid therapy within the employers health plan. The report identifies provders that are potentially over prescribing to plan members, which can increase healthcare encounters up to 3X greater than non-prescribed members. This initial analysis is provided at no cost, allowing health plans to verify if they have member re-fill patterns and provider prescribing patterns than can increase healthcare encounters up to 3X; increasing medical claims costs up to 15% each year.